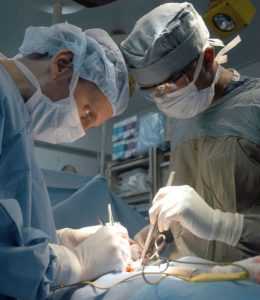
unnecessary spinal surgery
_ UNNECESSARY SPINAL SURGERYA PROSPECTIVE 1-YEAR STUDY OF ONE SURGEON’S EXPERIENCE In June of 2011, the medical journal Surgical Neurology International published a paper by
Mountain View, MO 65548
Call for an appointment
Closed 12:00 - 1:00

_ UNNECESSARY SPINAL SURGERYA PROSPECTIVE 1-YEAR STUDY OF ONE SURGEON’S EXPERIENCE In June of 2011, the medical journal Surgical Neurology International published a paper by

MONEY AND SPINAL SURGERYWHAT HAPPENED TO CARING FOR THE GERIATRIC PATIENT? Capri23auto (Ralph) – Deutschland – Pixabay In the April 2010 issue of JAMA (Journal

FREE OFFICE VISITADVICE: $50,000.00 Researchers recently searched 10 computer databases for clinical trials (the focus was on people with referred leg symptoms and MRI confirmation
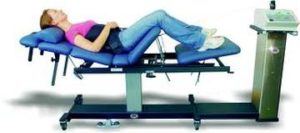
HOW MUCH DOES IT COST? The first step is to call (417) 934-6337 and schedule a free consultation with Dr. Schierling to find out WHETHER
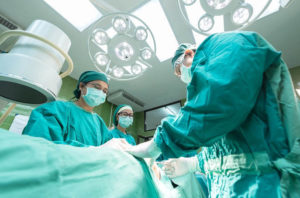
A Better Understanding of the Thoracolumbar Fascia Might Help You Prevent A Back Surgery! Dr. Helen Langevin is back as part of a yet another
PLASTIC SURGERY STARTS A DOWNHILL SPIRAL Every once and awhile, if I think a significant number of people might benefit, I take an email and
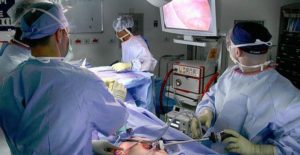
TOLD YOU NEED BACK SURGERY? THERE MAY BE A BETTER WAY “The rapid growth in spinal surgery volumes over the past 20 years has prompted
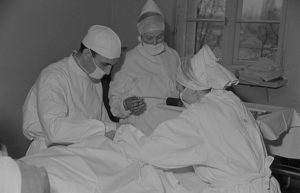
CURING BACK PAIN WITHOUT DRUGS OR SURGERY Roger Rössing / Quelle Deutsche Fotothek Look; FDA regulations being what they are, I would never myself use
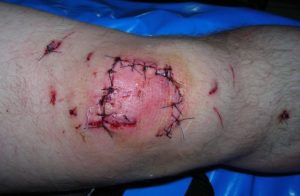
DOES KNEE SURGERY CAUSE KNEE ARTHRITIS?SEEMS SO “The meniscus is needed to distribute the body weight across the knee. Without the meniscus the body weight
“Cervical pain is one of the most common symptoms in today’s society. Indeed, in our personal clinical experience, well over 90% of patients with headache
HERNIATED OR DEGENERATIVE DISC, PIRIFORMISSYNDROME, OR ADHESED THORACOLUMBAR FASCIA? HERNIATED DISC PIRIFORMIS SYNDROME FASCIAL ADHESIONS “LBP [Low Back Pain] is the most expensive, benign condition

FAILED BACK SURGERY SYNDROME Bundesarchiv, Bild 183-40602-0005 / CC-BY-SA Most people I meet do not want SPINAL SURGERY. They realize that the majority of the
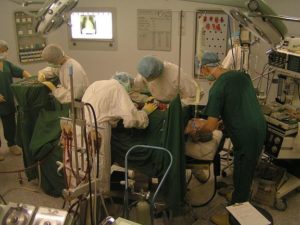
LOW BACK SURGERY?FAR LESS LIKELY FOR THOSE WHO USE CHIROPRACTIC FIRST Photo by Stefan Kühn Did you happen to hear about the series of seven
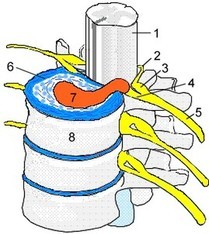
DISC HERNIATION?PIRIFORMIS SYNDROME? HERNIATED DISC PIRIFORMIS SYNDROME If you’ve ever had sciatica, you know what a nightmare it can be. Sciatica can range from the
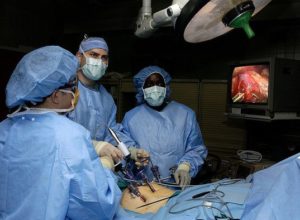
THINK TWICE ABOUT SPINAL SURGERY! Spinal Surgery is a leading surgical procedure in America, with the total number in the U.S. approaching half a million

Spinal Decompression -vs- TractionIs There a Difference? I have been asked numerous times about the difference between Traction and Spinal Decompression. Here is my 5

WHAT IF YOU LEARNED THAT HEALTH INSURANCE & WORKMAN’S COMP CARRIERS AND OUR GOVERNMENT WERE RESPONSIBLE FOR THE OPIOID CRISIS? Unless you’ve been living under
CHRONIC BACK PAIN AND FASCIAL ADHESIONS OF THE THORACOLUMBAR SPINEMIGHT THERE BE A SOLUTION FOR YOU? “The thoracolumbar fascia is thought to act as an

ROME’S DR. BRUNO BORDONI; EXPERT ON FASCIA AND IT’S RELATIONSHIP TO PAIN, DYSFUNCTION, AND DISEASE Although first touted by DR ANDREW TAYLOR STILL, there is
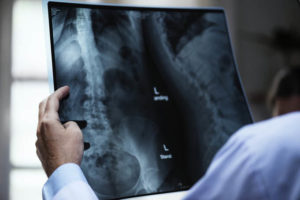
HALF THE ADULT AMERICAN POPULATION HAVE DISC HERNIATIONS WITHOUT LOW BACK PAIN – ANOTHER PROOF FOR THE THORACO-LUMBAR FASCIA MODEL OF LOW BACK PAIN “Spinal
Enter your name, email address and message in the box below to send us an email. If you’re in the Mountain View area, you can stop in to the office. We’re located in Mountain View at: 1219 South State, Route 17. Or, give us a call at: (417) 934 6337