
Fascial Adhesions Solved After a Fifteen Year Struggle with Neck Pain and Muscle Spasms
If you’ve ever skimmed over the surface of the crystal-clear CURRENT RIVER you share a bond with Molly. How so? Her family manufactures Blazer Boats
Mountain View, MO 65548
Call for an appointment
Closed 12:00 - 1:00

If you’ve ever skimmed over the surface of the crystal-clear CURRENT RIVER you share a bond with Molly. How so? Her family manufactures Blazer Boats

Although Cassie’s case was extremely common as far as what was wrong with her (FASCIAL ADHESIONS caused by SEVERE TRAUMA had caused unbearable neck pain,

The first thing I’d like to do today is apologize for not putting much new material up in the past month. We painted our house
POST-SURGICAL CHRONIC NECK PAINSOLVED IN A SINGLE VISIT! Imagine a life of CHRONIC UNRELENTING PAIN. Imagine a life lived from a PILL BOTTLE. Imagine

WHAT DOES THE LATEST RESEARCH ON NECK PAIN, HEADACHES, AND WHIPLASH REVEAL? “Neck pain is the most common musculoskeletal pathology second only to low back

COLORADO CHRONIC NECK PAIN RELIEFIN MOUNTAIN VIEW, MISSOURI To look at Kim the first time you meet her, not only would you not think

CHRONIC PAIN RELIEFUPPER BACK AND NECK It was nearly ten years ago that I first saw Anthony, who had come to me after he

FOUR-PLUS DECADES OF WHIPLASH PAIN SOLVED IN A SINGLE VISIT — FIVE YEARS AGO Carolyn is one of those upbeat people you can’t help

ADOLESCENT HAS CHRONIC NECK PAIN & HEADACHES FROM FALLING OUT OF A BARN LOFT ONTO HIS FACE…SOLVED IN ONE TREATMENT! I first met Tyler

Dan and I hit it off from the moment he walked into my clinic for his 6:30 am appointment. He had driven all the

Back in June a team of Swedish researchers put together a study for the Journal of Pain Research titled Exploring Patients’ Experiences of the Whiplash
FASCIAL ADHESIONS OF ANTERIOR MUSCLES CAUSE PAIN IN THE UPPER BACK AND NECK Any number of factors can come together to create a “PERFECT

LOOKING TO BREAK FREE FROM CHRONIC FIBROMYALGIA OR ARTHRITIS PAIN? TAKE CARE OF YOR ADHESED FASCIA! I’ve never bought a lottery ticket, but if

CHRONIC NECK PAIN FROM INJURED FASCIATISSUE REMODELING DRAMATICALLY IMPROVESTHE LIFE OF A LOCAL LOGGING ACCIDENT SURVIVOR In many ways TR has lived the life of

CHRONIC BACK & NECK PAIN: QUICK AND AMAZING RESULTS RULEA VIDEO TESTIMONIAL I’m not exactly sure when I first met Dean, but it was because

The Temporoparietal Fascia and Your Neck Pain and Headaches StatPearls describes itself as providing “peer-reviewed and PubMed-indexed review articles” created for the express purpose of

Muscle or Fascia Which is Responsible for Your Pain? When we look at the THREE TYPES OF PAIN, Type I (simple nociception) is not only
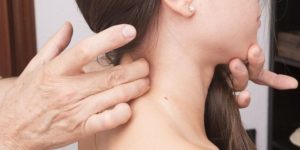
CHRONIC NECK PAIN?A SIMPLE SELF-TEST FOR HELPING DETERMINEWHETHER CERVICAL FASCIA MIGHT BE THE CULPRIT After describing the “paucity of soft tissue education” in our nation’s

CHRONIC NECK PAIN SOLUTIONS: ADDRESSING THE CHEMICAL, MECHANICAL, AND STRUCTURAL CAUSES OF PAIN When it comes to CHRONIC NECK PAIN there are three chief

According to Webster’s, the definition of ‘Maintenance’ is “The act of maintaining: the state of being maintained: support. The upkeep of property or equipment.” Wikipedia
Enter your name, email address and message in the box below to send us an email. If you’re in the Mountain View area, you can stop in to the office. We’re located in Mountain View at: 1219 South State, Route 17. Or, give us a call at: (417) 934 6337