
Fascial Adhesions Solved After a Fifteen Year Struggle with Neck Pain and Muscle Spasms
If you’ve ever skimmed over the surface of the crystal-clear CURRENT RIVER you share a bond with Molly. How so? Her family manufactures Blazer Boats
Mountain View, MO 65548
Call for an appointment
Closed 12:00 - 1:00

If you’ve ever skimmed over the surface of the crystal-clear CURRENT RIVER you share a bond with Molly. How so? Her family manufactures Blazer Boats

Although Cassie’s case was extremely common as far as what was wrong with her (FASCIAL ADHESIONS caused by SEVERE TRAUMA had caused unbearable neck pain,
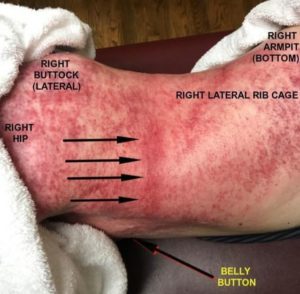
TORN OR ADHESED FASCIAWHAT IN THE WORLD DOES IT LOOK LIKE? Invisible. At some point in their life, everyone has secretly (or maybe not

When Paden came to see me last week for his second visit (his first was sometime in September of last year), he refreshed my memory

YOUR CHRONIC PAIN MAY NOT BE “CENTRAL SENSITIZATION” AFTER ALL “I have so much fascia pain all over due to a signal change in my
FASCIAL ADHESIONS OF ANTERIOR MUSCLES CAUSE PAIN IN THE UPPER BACK AND NECK Any number of factors can come together to create a “PERFECT

MECHANICAL THRESHOLD & ADHESED FASCIA WHAT YOU NEED TO UNDERSTAND IF YOU HOPE TO IMPROVE YOUR CONDITION Jump online, do a Google search, and you’ll

SYSTEMICALLY ADHESED FASCIA AND CHRONIC NAUSEA “Nausea and vomiting are among the most frequently occurring symptoms observed by clinicians. The involvement and importance of vagal
I frequently get emails like THIS ONE (people whom, unfortunately, I cannot help). I also get a lot of can-you-help-me requests from people who have

Fascial Adhesions: Deal With Them or They Will Deal With You! Inflammation presents a conundrum to friction-free fascia. On one hand it’s critical for normal

ANOTHER WAY TO DESTROY FASCIAL ADHESIONS When I say I used to be a powerlifter, I don’t mean that I was really a powerlifter, and
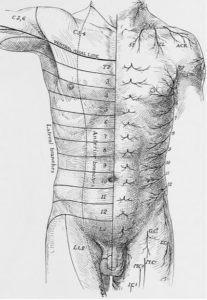
FASCIAL ADHESIONS, CHRONIC PAIN, AND CUTANEOUS NERVE ENTRAPMENTS: MORE COMMON THAN YOU EVER DREAMED! I’ve talked at length here about the way that SCAR TISSUE

CHRONIC HIP FLEXOR PAIN AND FASCIAL ADHESION IN A MIDDLE AGED WOMAN CHRONIC PAIN. It’s a bummer. The kicker is that some experts say that
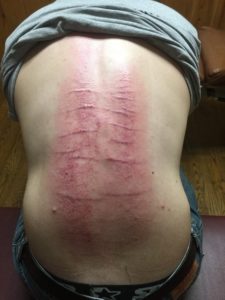
SCAR TISSUE, STRETCHMARKS, FASCIAL ADHESIONS, CHRONIC PAIN, AND CHRONIC RESTRICTION; KELOIDAL SCARS -vs- HYPERTROPHIC SCARS Let
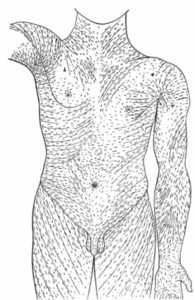
ADHESIONS OF THE FASCIA & LANGER’S LINES OF CLEAVAGE Not being a surgeon; until a few years ago I

SCAR TISSUE OR FIBROSIS?(THE MICROSCOPIC STRUCTURE OF SCARRED FASCIA) NORMAL TISSUE SCAR TISSUE In my last post (HERE), I
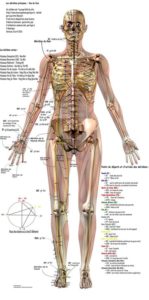
Although the term “Dry Needling” was coined by Dr. Janet Travell in her Magnus Opus (Myofascial Pain and Dysfunction: Trigger Point Manual), it has been
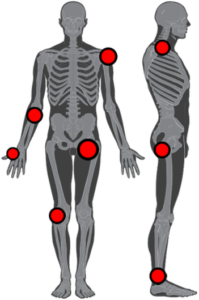
TENDINITIS OR TENDINOSIS?IT DOESN’T MATTER WHEN IT COMES TO ICD-10 Patrick J. Lynch; illustrator; C. Carl Jaffe; MD; cardiologist “Confusion between Tendonitis versus Tendinosis: Tendonitis

FASCIAL ADHESIONSA COMMONLY OVERLOOKED CAUSE OF CHRONIC PAIN Annemarie Busschers I well remember an incident that happened while in Anatomy Class back when I was

ADHESED FASCIA IN CHILDRENMORE COMMON THAN YOU MIGHT SUSPECT In response to YESTERDAY’S POST on childhood headaches, I had someone drop me an email accusing
Enter your name, email address and message in the box below to send us an email. If you’re in the Mountain View area, you can stop in to the office. We’re located in Mountain View at: 1219 South State, Route 17. Or, give us a call at: (417) 934 6337